Human chorionic gonadotropin
Human chorionic gonadotropin (hCG) is produced by the placental syncytiotrophoblast and first appears in maternal blood 10 days after fertilization. It peaks at 9–10 weeks and then gradually falls to a plateau level at 20–22 weeks.
By chemical structure hCG is a glycoprotein with 2 subunits. The α-subunit is similar to luteinizing hormone (LH), follicle-stimulating hormone (FSH), and thyrotropin (TSH). The β-subunit is specific for pregnancy.
The functions of hCG are as follows:
- Maintain corpus luteum production of progesterone until the placenta can take over maintenance of the pregnancy
- Regulate steroid biosynthesis in the placenta and fetal adrenal gland as well
- Stimulate testosterone production in the fetal male testes
If hCG levels are high, twin pregnancy, hydatidiform mole, choriocarcinoma, or embryonal carcinoma can occur. If levels are low, ectopic pregnancy, threatened abortion, or missed abortion can occur.
Human placental lactogen
Human placental lactogen is chemically similar to anterior pituitary growth hormone and prolactin. Its level parallels placental growth, rising throughout pregnancy.
Its effect is to antagonize the cellular action of insulin, decreasing insulin utilization and thereby contributing to the predisposition of pregnancy to glucose intolerance and diabetes.
If levels are low, threatened abortion or intrauterine growth restriction (IUGR) can occur.
Progesterone
Progesterone is a steroid hormone produced after ovulation by the luteal cells of the corpus luteum to induce endometrial secretory changes favorable for blastocyst implantation.
It is initially produced exclusively by the corpus luteum for up to 6–7 menstrual weeks. Between 7–9 weeks, both the corpus luteum and the placenta produce progesterone. After 9 weeks the corpus luteum declines, and progesterone is exclusively produced by the placenta.
It is initially produced exclusively by the corpus luteum for up to 6–7 menstrual weeks. Between 7–9 weeks, both the corpus luteum and the placenta produce progesterone. After 9 weeks the corpus luteum declines, and progesterone is exclusively produced by the placenta.
The functions of progesterone are as follows:
- In early pregnancy it induces endometrial secretory changes favorable for blastocyst implantation.
- In later pregnancy its function is to induce immune tolerance for the pregnancy and prevent myometrial contractions.
Estrogen:
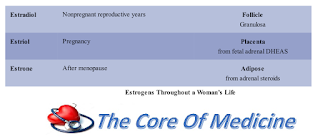
Estrogens are steroid hormones that occur in 3 forms. Each form has unique significance during a woman’s life.
Estradiol is the predominant moiety during the nonpregnant reproductive years. It is converted from androgens (produced from cholesterol in the follicular theca cells), which diffuse into the follicular granulosa cells containing the aromatase enzyme that completes the transformation into estradiol.
Estriol is the main estrogen during pregnancy. Dehydroepiandrosterone-sulfate (DHEAS) from the fetal adrenal gland is the precursor for 90% of estriol converted by sulfatase enzyme in the placenta.
Estrone is the main form during menopause. Postmenopausally, adrenal androstenedione is converted in peripheral adipose tissue to estrone.